 Eventually, after electric pulse treatment two stones, broke down and I passed them in my urine. I was given an appointment for July 2012 for review. In July, I went for a scan and the doctor in charge said I had something seriously wrong since she could see a “fog” or liquid around my liver and my spleen. She advised me to go back to the hospital immediately.
Eventually, after electric pulse treatment two stones, broke down and I passed them in my urine. I was given an appointment for July 2012 for review. In July, I went for a scan and the doctor in charge said I had something seriously wrong since she could see a “fog” or liquid around my liver and my spleen. She advised me to go back to the hospital immediately.
That afternoon I say the doctor who had treated me while in hospital and he confirmed that this liquid had been there on the first scan taken in June. He said it was probably due to inflation caused by the kidney stones and told me to wait for another three months and have an Ultrasound (a scan was considered too expensive).
At the beginning of November 2012, I went for an ultrasound and again the doctor said there was something abnormal and told me to have a scan. I had the scan the following month and I saw the consultant Doctor Crampon in January 2013. The doctor in charge of the scan and my consultant still did not know what this liquid was. They did not think it was a cancer but they really had no idea.
An endoscopy was organised and two procedures were done – both “up and down”. The consult confirmed that there was no sign of cancer in the stomach or in the intestines. A lesion was found and removed as part of the procedure.
At that point, the consultant decided to refer me to the oncology department at the CHU Estaing hospital in Clermont-Ferrand, France (Pole Digestif Hépatobiliaire). There I met a Professor Pezet and on inspection of the scan he suggested I had a condition called pseudomyxoma peritonei (PMP). He explained that it was a type of cancer but to be sure he would do a biopsy.
The biopsy was organised and it was to be carried out laparoscopically. I was in hospital for 4 hours and 4 insertions were made. The operation lasted 40 minutes. I was discharged the same day with a prescription for pain killers which came in useful since I was off work for 4 days because of the pain after the operation. A further appointment was organised to discuss the results and it was confirmed I had PMP. That was for April 15th, 2013.
Mucin had been found around the spleen, the liver and as far down at the Douglas cavity. A series of nodules had been found attached to the intestines and it was explained to me that part of these would have to be removed. The Professor explained that he could not confirm the severity of the problem until I was opened up but did tell me that the worst scenario would be two operations:
- The removal of the mucin, body parts and perhaps part of the colon/intestines.
This could leave me with a colostomy for 2 months at which stage the procedure could be reversed. In addition, I would be given chemotherapy called heated intra-peritoneal chemotherapy (HIPEC) at the same time as the operation in order to “burn” any remaining cancerous cells. It was explained that this was done for approximately 90 minutes. - The reversal procedure to reconnect the intestines
I was told it would take me four months to recuperate. All in all it took eight months to diagnose but once I saw a cancer specialist in February 2013 the diagnosis had been immediate, barring confirmation. The official date of confirmation was the 26/03/2013 when the report was written and I was told the 15/04/2013. I was 59 years old at time of confirmation.
I was initially given a date of the June 3rd 2013 for my operation but this was delayed by one week. Here in France, work is assessed on a priority basis with patients normally given the week of the operation but not the date until the Friday before. At this stage, they decided to delay and give me a new date a week later.
On the following Friday, I was given a date of entry of June 9th 2013. On entry that day they asked me to shave and scrub myself. I prepared myself that night by shaving from just above my biceps down to the groin.
I was wheeled into the preparation theatre at 8.00am on June 10th 2013 and the anesthesiologist tried to give me an epidural – it seems this was not successful but I do not know since I passed out.
That afternoon, after an operation lasting eight hours, I was transferred to Intensive Care. I had two drains, one on the left and right for my abdominal cavity.
The next day it was explained to me that I had had my appendix removed, part of the liver removed, all of the mucin. All the organs in the cavity were scrapped in order to ‘clean’ them. In addition, I had also had part of my intestine removed but the good news was the cancer was not advanced as initially thought and I did not have a colostomy. Thus no need for a second operation.
I was in intensive care for five days. I had a multitude of different medicines fed by a drip and these were progressively removed during that time.
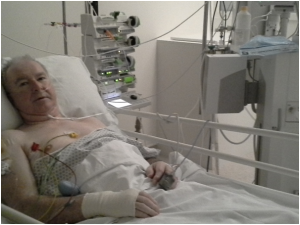 The first night I asked to go to the toilet but was told it was okay since I had a catheter inserted in my penis. Strange sensation!!!
The first night I asked to go to the toilet but was told it was okay since I had a catheter inserted in my penis. Strange sensation!!!
The second day I was asked to get out of bed to move around and this was possible for 15 minutes. I tried to eat something but I just felt nauseous all the time.
The third day it was found I had fluid on my lung and another drain was inserted – this was the most painful experience during that first week.
Again I was not feeling hungry and ate hardly anything. Because of the third drain, I was not able to get out of bed. The fourth and fifth days were similar – I did not get out of bed and hardly ate anything.
During the time in intensive care, I had an X-ray every day and a bed-bath every day. My stitches were inspected and treated every day. On the fifth day, they were left open to allow air to get to them. In all, I had 44 metal staples on the outside and I was told about 80 stitches on the inside.
I was lucky in that during those five days I was in intensive care I did not have to evacuate my bowels thus allow the healing process to continue unheeded. The downside is that I lost over 14 pounds during that time.
Because of the constant pain, I found it difficult to sleep and was on self-medication (morphine drip) during this time. The dreams I had were weird, it was almost like an out-of-body experience.
At the end of the fifth day, I was transferred to the ward which was a private room. The X-rays continued every day and I was allowed to stay on morphine for another three days at which time the drip was removed. I was questioned every day as to the level of pain and feeling and my medication was adjusted accordingly.
I was able to evacuate my bowels for the first time on the sixth day. I could not face the hospital food and my wife would bring in for me two meals a day (I did eat the bread and jam in the morning). Even then I could not face a full meal because of nausea.
By the end of the ninth day, the anesthesiologist suggested I have a tube inserted so that I could be fed with vitamins to supplement my diet since I was losing weight. I suppose a little like ‘foie gras’ and force-feeding. This was horrendous since my throat was already swollen from the operation and I was heaving all of the time. After two hours, I started to vomit and it was decided to remove the tube.
By the end of the tenth day the first drip was removed – the one from my lung– this was an enormous relief because this constantly give me pain. By the end of the eleventh day, the second drip was removed. By the morning of the thirteenth day, the third drip was removed and I was discharged the same day!
Over the next ten days following my discharge from the hospital, I was visited by the district nurse and the doctor twice. I had had problems with my back and could not get comfortable. It was suggested I had something called ‘Table syndrome’ which was due to the time I had spent on my back during the operation and in intensive care and the hospital ward (being that it was impossible to lie in any other position than on my back).
 The doctor instructed my wife in how to massage my back and this became indispensable since every time I ate I also ended up with indigestion even though on medication.
The doctor instructed my wife in how to massage my back and this became indispensable since every time I ate I also ended up with indigestion even though on medication.
The district nurse would tend to my dressings and also inject me every day with an anti-coagulant.
By the end of the third week after the operation, the staples were removed in two stages to ensure the wound did not rupture. I was told to cream the wound everyday. I never had any problem with the wound and still cream the scar after several months.
One further complication was gout. I have suffered from gout for 13 years. I have not had a major crisis in over 6 years and I am on daily medication. During the first 10 days in hospital I was not allowed to take the medication and by the third week I had started to experience severe gout. This lasted for a further 3 weeks. I was already suffering from diarrhoea and the crisis medication always brings on diarrhoea therefore I was still losing weight during this period and I could not walk. The doctor came to see me and prescribed a different treatment which in reality was no better.
Eventually, this subsided and I was able to exercise and start to move. I had problems with shortage of breath, back ache (as explained), nausea, diarrhoea, stomach pains and also I found it difficult to urinate.
This last issue was a reason for me visiting the doctor. He thought it was a urine infection. I was sent for an ultrasound but this confirmed it was not. Unfortunately, the doctor doing the ultrasound could not see all of the organs because of the inflammation and I thought we were still talking of liquid in the abdomen. Eventually, after 5 weeks this subsided and now it is fine.
Concentration was also a problem; I was able to watch television but reading was a problem as was trying to do anything on a computer.
In August, I returned to see the Professor. He was just interested to see my general health since he had nothing really to go on since I had not been scanned. The whole thing just took 15 minutes and we arranged a scan for the November and a follow-up appointment for five days after that.
On the November 12th 2013, I was told that the scan showed that everything was clear – Thank God!! – But also thanks to the professionalism of the French team – I cannot fault them at all, from the district nurses all the way to the Professor himself. Professor Pezet has now booked another scan in 6 months’ time.
I still have problems with my bowels but this is gradually improving. I had prepared myself for a recovery time of five weeks. I never anticipated three to four months.
I had problems sleeping. Because I was laying on my back for so long and could not get comfortable, I slept on the couch for four weeks. Each time I tried to go back to bed I would wake at about 2.00am and that would be it for four hours. Even when I decided to try bed again it was a separate bed because I did not want to disturb my wife. It took three months before I got back to normal.
I think some of these issues were also related to frustration – not being my normal self and no matter what my wife or friends or the doctor said – it did not make it feel better. The saying “only time can heal” is true.
What do I feel now? LUCKY!!!
Knowing that this is a silent killer, I was in the right place at the right time.
- The fact that I had kidney stones – with all its pain – really helped me out because without them it is highly unlikely I would have been diagnosed
- The fact that I lived in Clermont-Ferrand – one of the two major centres in France for this treatment – was fortuitous
- The fact that I live in France with an exceptional health service meant that once diagnosed the time for reaction was weeks. Also the persistence of the consultants meant I was progressed on a regular basis
What advice could I give to others?
Get a body scan!! We do not know what is in our body sometimes. We feel pain, we can feel growths but that does not tell us exactly what is happening; I would advise anybody now to get a scan at 45 and 55 and invest in this form of diagnosis.
In terms of cancer support – this is a hard question? I preferred to go it “blind”. I did not want to read all of the dialogue or information on the subject. I read a few of the survivor’s stories just to see if there was really a survival rate. I also believed in my doctor who told me they could treat it and that most likely I would survive. You have to have that trust.
I think people should seek out advice and advisors should judge what to say based on the emotional state of the person in question. The doctor has already told the patient the problem – the patient now needs support in whatever form through the period of time. My advisor and councillor was my wife – she was there to listen; there to give a response and there to make me feel secure. Not all people are capable of this support which is why a network of experience is required.
– John
In case you missed it...
My pseudomyxoma peritonei was discovered during a proctocolectomy
My PMP was discovered during a proctocolectomy¹ for what was thought to be an uncontrollable flare-up of Ulcerative Colitis.
I’m now on ‘watch and wait’ following a diagnosis of pseudomyxoma peritonei
For me, it all started with blood in my urine and an increase in the size of my stomach. In retrospect, I could feel the mucin moving when I walked. Now I’m on ‘watch and wait’.
Diagnosed with pseudomyxoma peritonei when I was pregnant
Lauren was diagnosed with PMP following her 20-week prenatal ultrasound.




John, thank you so much for your story. You offer very good advice. I was diagnosed and treated 2007, and am doing well. However, I have had kidney stones twice since my operation. I have read that any type of gut altering surgery can increase the chances of kidney stones. I suspect that this is my case.